Inside the Invader
The making of a pandemic and what we can do about it
 Dhrubaa Ghosh
Dhrubaa Ghosh
 Dhrubaa Ghosh
|
20 Mar, 2020
Dhrubaa Ghosh
|
20 Mar, 2020
/wp-content/uploads/2020/03/Insidetheinvader1.jpg)
Coronavirus COVID-19, a glass sculpture by Luke Jerram (Photo: Getty Images)
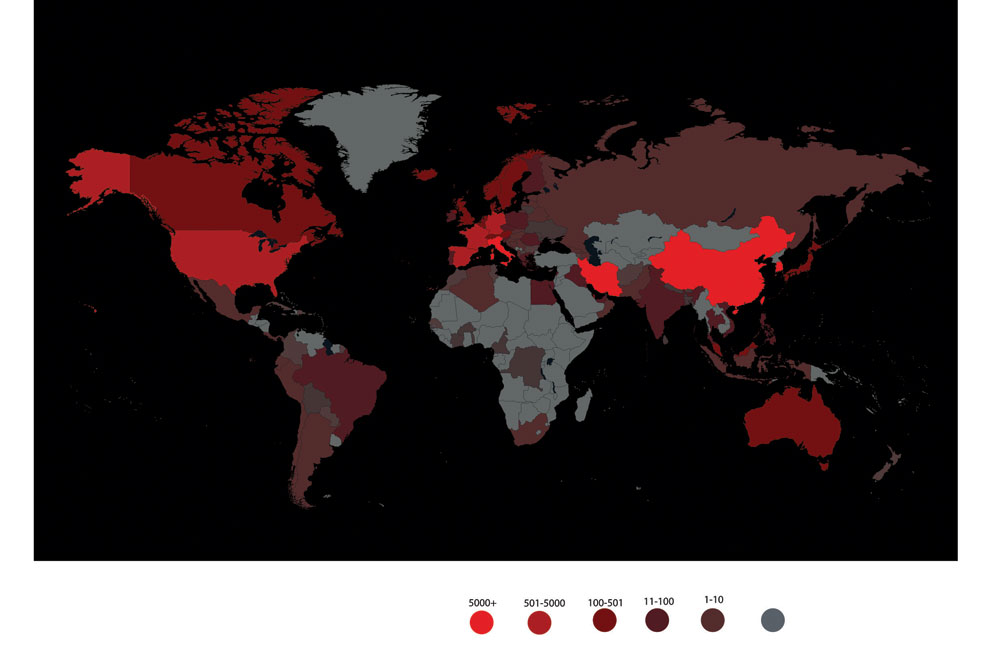
The ongoing Covid-19 outbreak has been declared a pandemic by the World Health Organization (WHO). As of March 16th, the United Nations’ public health agency has confirmed 167,511 cases, including 6,606 fatalities across 151 countries around the world. As countries begin shutting down borders, cutting off international trade and quarantining their populations, the key to protect our families and communities lies in understanding the nature and behaviour and why and how this particular virus is spreading.
At the core of the current global public health emergency is a highly contagious virus with spherical particles spanning just a few nanometers in size that cause illnesses ranging from common cold to Severe Acute Respiratory Syndrome (CoV-SARS).
Human coronaviruses have existed before—229E-like and OC43-like, NL63 and HKU1—but this one, the particular strain SARS Coronavirus 2, is novel. This coronavirus manifests in the human body as a respiratory infection, showcasing symptoms very similar to the common flu. ‘Corona’ actually refers to halo or crown-like projections that are observed on the outer side of the virus and are found in avian and mammalian species, but there is no definitive evidence so far that human coronaviruses can be transmitted by animals.
Coronavirus infections (though not specifically Covid-19) are more common than you think. In fact, about one in five colds is due to coronavirus, as waves of infection pass through the community during winter months. Only about one-third to half of infected individuals develop symptoms. Because coronavirus infections are common, many individuals have specific antibodies in their nasal secretions, and these antibodies can protect against infection. Most of these antibodies are directed against the surface projections or the corona, and neutralise the infectivity of the virus.
To understand how this virus spreads, we must peek inside the shell of the virus. Here, we’ll find genetic material called RNA, which helps the virus replicate and mutate very quickly. This virus is transmitted through airborne droplets to the nasal mucosa, or the lining of the nose. So all it takes to pass on the infection is a cough, sneeze, or even a runny nose. Shared surfaces are also particularly risky since the virus clings on to surfaces and propagates as soon as another person touches the shared surface. It can remain active for about three hours after aerosolization (droplets carrying virus mixed with air), on metallic surfaces for 5-6 hours, and on plastic for 15 hours. But do note that the average immune system doesn’t go down without a fight: It takes a large number of virus particles to break down a healthy immune system; so making contact with surfaces infected with the virus may not necessarily make a person sick.
Covid-19 has an incubation period of three days and shows the symptoms we typically associate with the common cold—including nasal obstruction, sneezing, runny nose, fever and the occasional cough. The cell damage triggers inflammatory mediators, which gives the host a runny nose with inflammation and swelling. There is also some evidence that the respiratory coronaviruses can cause disease of the lower respiratory tract, but it is unlikely that this is due to direct invasion.
Currently, Remedesivir by Gilead Sciences is the only available drug with demonstrated efficacy in treating Covid-19 in China, with ongoing trials in Italy
Advancements in the field of genetic engineering and technology have also made it possible to sequence the new coronavirus, that is, read the virus’ genetic material with precision to identify it as Covid-19. Diagnosing the Covid-19 strain requires bespoke testing tools, in particular, a laboratory test called RT-PCR. Conducted on the throat or nasal swab, this test detects the genetic material of the virus. The test’s results are subsequently reconfirmed by a method called ‘gene fingerprinting’. Developed using genetic engineering and molecular methods, these tests have demonstrated high accuracy rates when samples have been collected properly.
Results from genetic sequencing of Covid-19 allows public health authorities to establish the length and provenance of the virus. It allowed researchers to pinpoint the earliest case in Wuhan, China, on November 17th, 2019, and discover its ability to propagate so quickly and surreptitiously. Genetic sequencing also reads changes in the virus’ genetic material, like mutations, which can provide salient insights as we develop diagnostic tests and continue to search for treatment.
At the same time, many public health professionals, including virologists, believe that the virus has been able to spread so quickly while evading detection from authorities because critical tests haven’t been very accessible. Though currently used diagnostic methods and hardware are reliable, they are costly, time-consuming and require a specialist’s skillset to administer. Thus, they aren’t very accessible to most research laboratories or public health agencies, hamstringing screening processes from keeping pace with the contagion.
What makes Covid-19 even more insidious is its pre-symptomatic nature: While reports put Wuhan as ground zero of the outbreak, it has been difficult to pinpoint and detect its proliferation within a highly mobile global population because many hosts didn’t show a single symptom even while they were carrying the virus. This is also how the virus, in its early onset period, efficiently slipped into different geographies, including Italy, Iran and Spain, which are now reporting the highest number of cases.
In terms of responses to this pandemic, public health authorities have broadly followed two key approaches. The first approach, adopted by countries like China, Italy and Singapore, involves enacting drastic measures to minimise human interaction. This includes social distancing, full-scale lockdowns and travel bans. In France, for instance, authorities have ordered people to confine themselves to their homes and closed restaurants, bars and other non-essential businesses.
The more ‘alternative’ method of containing the spread, initially being championed by the UK and Ireland authorities, consisted of achieving ‘herd immunity’. Having monitored the experiences of Singapore and China, the UK government opted against extreme containment measures, focusing on exposing segments of its population to the virus with the intention of bolstering general resilience to the virus as and when it resurfaces in the future (winter season). However, considering the ethical costs of such a tactic—scientists discovered that this approach is only effective when 60 per cent of the population is infected, making for a sizeable caseload that could potentially break the National Health Service—prompted the UK government to nix the strategy.
ON THE TREATMENT front, there are no specific antivirals or vaccines against the Covid-19 strain of coronavirus, but there is hope: researchers are trialing antiretrovirals to treat coronavirus infections. These drugs are similar to those used for treating HIV patients—they work by blocking a key enzyme that stalls the virus’ ability to replicate. While these drugs were found to alleviate the impact of previous outbreaks of coronavirus, it should be noted that they were only used in severe cases, commonly seen in ICUs and not for any coronavirus-positive case. Currently, Remedesivir by Gilead Sciences is the only commercially available drug with demonstrated efficacy in treating Covid-19 in China, with ongoing trials in Italy.
On a practical level, the need of the hour is to contain the spread through proper practices. For starters, it is important to read and follow instructions announced by the WHO (check their social media handles). Underscored by the Government, there are practical steps you can take—avoiding public places, maintaining social distance and personal hygiene to avoid compromising your body’s immune system, which in turn, reduces your vulnerability. In mild cases, the virus has been seen to clear out through adequate hydration, rest and nutrition.
Washing hands thoroughly with soap water also offers a robust first line of defence because it helps break down the outer coat of the virus, inhibiting its ability to attach to host cells. Similarly, coughing into the sleeves of your jacket can prevent dissemination of the virus from hands. Capturing the virus in fabric also threatens its very survival. Once infected, the body’s natural defence mechanism also kicks into top gear, generating antibodies against the virus and recovery is expected within 3-4 days (in case of mild infection). However, on the fifth day, symptoms of shortness of breath may appear due to the reaction of the body to the virus.
There are lessons to be learned from the coronavirus pandemic. For one, no pandemic or epidemic offers a notice period before infecting a population. Thus it is important to be prepared at scale: every country, at the very least, should have detection kits for mass screening and institute an emergency taskforce that is ready and trained to inform policymaking under times of duress.
Additionally, it is important to recognise and prepare for the heightened risk unique to developing countries. A country like India, for instance, can’t expect to confine transmissions to zero when its very population is a staggering 1.3 billion. More importantly, the country’s social, economic and public health circumstances amplify the risk of fatality not just among the elderly, but also among segments saddled with a litany of other pre-existing conditions, including malnutrition, TB, smoking, asthma and respiratory distress due to air pollution. Thus, these outstanding health vulnerabilities need to be addressed urgently, if we are to improve our population’s collective resilience.
Another underrepresented factor in exacerbating the impacts of viral outbreaks is climate change. Erratic swings in temperature and increased emissions of greenhouse gases facilitate the ambient conditions necessary to generate novel viral infections and reprise past outbreaks. Formulating actionable policies that recognise such interdependencies is the first step countries can take towards reducing the likelihood of such viral outbreaks in the future.
In today’s globalised world with its set of highly networked, interdependent economies, deadly infections can transcend national boundaries within hours and demonstrate what scientists call “exponential growth”. Tackling such challenges necessitates international cooperation and co-investment in instituting and maintaining a shared, robust public health infrastructure that comprises a powerful disease surveillance system to track and monitor emerging microbes and an assortment of effective and scalable healthcare delivery systems that minimise morbidity, mortality and expenses to those who need it.
Lastly, while we spend more time at home caring for our families, friends and colleagues, we must also give respect to the caregivers. It is the frontline public health workers who risk their own well-being in the field 24×7 to keep us safe. Most importantly, during an emergency, rumours and misinformation should be checked because they trigger diseases just as contagious and deadly as the coronavirus—paranoia, panic and stigma.
Click here to read all Coronavirus related articles

/wp-content/uploads/2025/06/Cover-OpenMinds2025.jpg)












More Columns
Puri Marks Sixth Major Stampede of The Year Open
Under the sunlit skies, in the city of Copernicus Sabin Iqbal
EC uploads Bihar’s 2003 electoral roll to ease document submission Open