Let There Be Light
Long-term lockdowns are not the answer to the virus
 Deepak Nayyar
Deepak Nayyar
 Deepak Nayyar
Deepak Nayyar
 |
15 May, 2020
|
15 May, 2020
/wp-content/uploads/2020/05/Light1.jpg)
(Illustration: Saurabh Singh)
THE OLDEST AND largest democracies in the world—the US and India, respectively—are often compared for striking differences and unexpected similarities. This time round, however, the difference that has surfaced would have been thought of as imagination running wild even three months ago. The first person tested positive for Covid-19 on January 21st in the US and on January 30th in India. More than three months later, on May 8th, the total number of infections was 1,323,000 in the US and 59,700 in India, accounting for 33 per cent and 1.5 per cent of the world total, while the number of Covid-19 deaths was 78,600 in the US and 2,000 in India, making up 28.5 per cent and 0.7 per cent of the world total. The share of the two countries in world population, by contrast, is 4 per cent and 18 per cent, respectively.
Before the pandemic, it would have been impossible to predict, let alone imagine, such a reality. Income per capita in India is a mere 3.2 per cent ($2,010) of that in the US ($62,800). About one-fourth of the world’s poor live in India, so that absolute poverty is high and nutrition levels are low. Population density in India is among the highest in the world. The poor, who live cheek-by-jowl in urban slums and cramped spaces in rural areas, are most susceptible to a virus that is contagious. Public health systems and facilities are perhaps among the worst anywhere. The US is a world apart.
The contrast stretches beyond the US. On May 7th, the cumulative total of Covid-19 deaths per million population in India was 1.3, as compared with 553 in Spain, 491 in Italy, 452 in the UK, 385 in France, 224 in the US and 88 in Germany. The corresponding figures were 6 in South Korea, 4.5 in Japan, 3.3 in China, 3.3 in Indonesia, 1.2 in Bangladesh, 0.8 in Thailand and 0.4 in Sri Lanka.
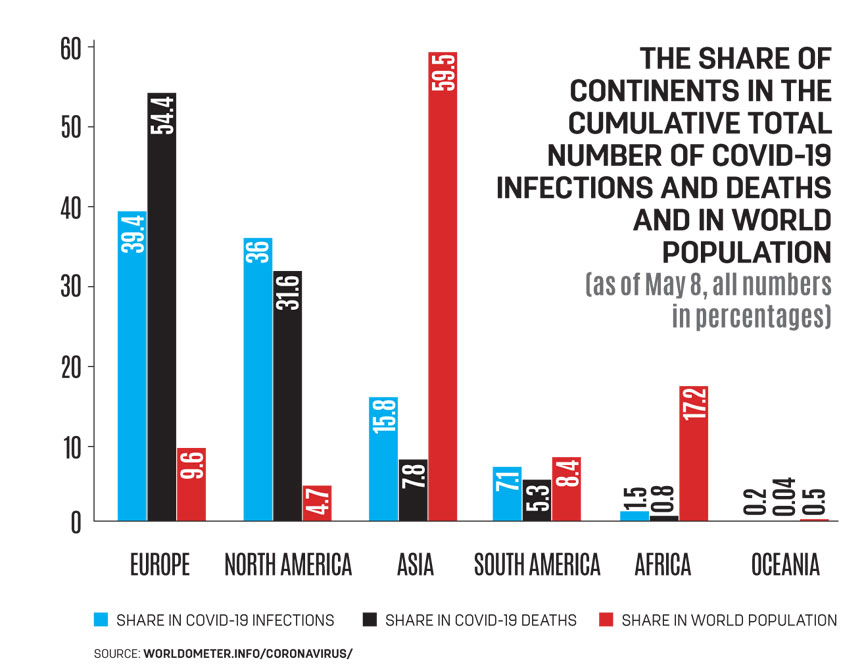
The asymmetry is even more striking if we consider the distribution of the Covid-19 infections and deaths by continent. On May 8th, in the cumulative totals, Europe and North America, taken together, accounted for 75 per cent of infections and 86 per cent of deaths in the world, although their share in world population is only 14 per cent. In sharp contrast, Asia accounted for 15.8 per cent of infections and 7.8 per cent of deaths, while its share in world population is almost 60 per cent. Africa accounted for only 1.5 per cent of infections and 0.8 per cent of deaths, though 17 per cent of the world population lives there. Compared with North America and Western Europe, or their own population size, the number of infections and deaths in India, as well as Asia and Africa, is far lower. The outcome, then, is puzzling if not paradoxical. Indeed, there is an irony here. Of the worldwide Covid-19 deaths, almost 90 per cent are in rich industrialised countries, whereas just over 10 per cent are in poor developing countries, which are the proverbial home of disease and death (see chart).
Of course, it is plausible to argue that, unlike the rich countries, India is in the early stages where community transmission has not gathered momentum, so that an explosive growth in infection numbers could yet surface later, or in a second round.
How can we explain this situation in which, so far, India has fared better than many other parts of the world? Past experience of the Spanish influenza in 1918, when India accounted for 18-20 million of the estimated 50 million deaths in the world, or conventional thinking even now, would have led to the opposite conclusion. There are two possible explanations.
First, the reality might be much worse than the statistics suggest because the total number of infections is almost certainly underestimated, as testing has been nowhere near enough, given the scarcity of testing kits and the massive population. Improved statistics might change the numbers but cannot transform the asymmetry.
Second, the lockdown imposed by the Government in India straddling its vast geography, perhaps the most stringent in the world, could have made a difference. The purpose was to break the chain of transmission through social distancing, which has two dimensions. For one, it confined people to their homes. But this created physical distancing only for the privileged living in homes that have spaces and doors. It was impossible for people in urban slums in megacities, where migrant workers also lived, often as many as 10 to a room. For another, it meant that people could not move within cities or across states, while migrant workers could not return to their villages. This did strangle potential chains of community transmission, even if only in part, reducing the geographical spread of the virus through contagion compared with what it would have been without a lockdown.
For governments, imposing and continuing lockdowns is a risk-averse strategy. If the spread can be restrained and manned, the success would bring political dividends. If the spread continues unabated or worsens, the microbe would take the blame for the failure
This obvious explanation is necessary but not sufficient because other countries which have imposed lockdowns, say, in Western Europe, with public health systems that are far superior, have not managed to slow down the phenomenal spread in the number of infections as much.
The reality that has unfolded so far, not just in India, but also in Asia and Africa, compared with North America and Western Europe, is puzzling and deserves some explanation. I am not an epidemiologist or a virologist. But as a social scientist, it is possible to observe outcomes which are counter-intuitive and think about plausible hypotheses.
The impact of diseases can and does differ across countries and continents, possibly attributable to differences in demographics, geographies, climates, cultures or immunities. Asia and Africa have much younger populations than Europe and North America, which could explain lower morbidity and mortality. Geographies shape climates, mostly tropical in Asia and Africa and mostly temperate in the West. It seems that Covid-19 has ravaged Western Europe and the US, while Asia and Africa, where malaria has been widespread in the past, are relatively unscathed. Anthropologists might reflect on whether or not cultural differences matter. Scientists or immunologists could investigate how or why immunities differ. Much of this is largely unexplored so far.
It has been suggested that countries that have mandatory BCG vaccinations against tuberculosis are less susceptible to Covid-19 morbidity and mortality. Compare, for example, the Iberian Peninsula countries, Spain and Portugal. On May 8th, Spain had around 260,100 infections and 26,300 deaths, whereas Portugal had 27,300 infections and 1,100 deaths. Is it only a coincidence that BCG vaccinations are mandatory in Portugal but not in Spain, or that the US and Italy, both ravaged by Covid-19, never had universal BCG vaccination programmes? Obviously, it is only scientific investigation that can establish cause-and-effect.
Research suggests the BCG vaccine seems to have a stimulating effect on the immune system that goes well beyond tuberculosis. Similar results have been derived from research on the polio vaccine. The inference drawn is that these vaccines reduce overall mortality more than would be expected through their effects on the diseases they are meant to prevent. The conventional assumption is that vaccines create antibodies against specific pathogens. But immunologists have discovered that live vaccines also stimulate innate immune systems creating capacities to better resist, or fight, other kinds of pathogens too. This idea of immune system protection, against multiple pathogens, is being explored by immunologists.
For that reason perhaps, some countries are running trials of BCG and polio vaccines against Covid-19, or thinking of these as a means of protecting health workers. Similarly, countries are buying hydroxychloroquine in large quantities from India, as a prophylactic for health workers. In India, BCG and polio vaccination is mandatory, while people’s immune systems have a lifelong exposure to curative and preventive drugs for malaria.
Such factors, implicit in demographics, geographies, climates or immunities, could provide possible explanations for the relatively limited impact of Covid-19 in India as well as several countries in Asia and Africa so far, when compared with countries in North America and Western Europe.
The draconian nationwide lockdown in India began on March 25th and completed 40 days on May 3rd. It was extended further until May 17th, with some relaxation in districts that have not had any infection so far, or any new infection in the past 21 days. However, these districts account for just about one-fifth of economic activity in the country, and resumption is easier said than done in a situation where there is a complex web of restrictions and supply chains are disrupted. Moreover, the lockdown could continue for longer, as there is no downturn yet, and the flattening curve is threatening to rise again, even if 80 per cent of the spread is concentrated in a few cities and states.
For governments everywhere, more so after the experience of Italy, Spain, the UK and the US, where governments did too little, too late, imposing and continuing lockdowns is a risk-averse strategy. If the spread can be restrained and managed, the success would bring political dividends. If the spread continues unabated or worsens, the microbe would take the blame for the failure. It is the equivalent of a one-way option in financial markets, tempting political leaders to think that they cannot lose. It is no surprise that in consultations with the Prime Minister, so many chief ministers have urged that the lockdown should continue. This is even more attractive now as it conforms to herd behaviour by governments worldwide. Exit from a lockdown, then, poses a real dilemma for governments. It calls for decision-making under high uncertainty, requiring courage that needs both conviction and confidence.
This dilemma becomes larger than life when governments emphasise saving lives in a pandemic as their primary, if not sole, objective. The objective, in itself, is unexceptionable. But it must also be recognised that the health of people and of an economy are interdependent, where both, taken together, shape the wellbeing of people. Thus, saving livelihoods is an equally important objective. The relationship between lives and livelihoods is circular. If lives are saved and, in doing so, livelihoods are sacrificed, it threatens the lives of people who are deprived of incomes and hence unable to meet their basic human needs. This could lead to widespread hunger, reduced immunity and lost lives. Obviously, getting sick and going hungry cannot be an either-or choice.
Everyone would want to stay healthy and be well fed. It is the role of governments to strike a balance and reconcile these two objectives, rather than juxtapose them as conflicting.
The lockdown has shut down almost two-thirds of the economy and the collateral damage is enormous. It stranded 25-30 million migrants in cities far away from their homes, deprived of their work and dignity, at the mercy of shelters for food provided by state governments or charities, often hungry and homeless. Manufacturing, mining, construction, trade, hotels and restaurants, and transport, which account for more than 40 per cent of both output and employment, were shut down completely. Thus, 150 million people, as much as one-third of our workforce, who are casual labourers on daily wages or workers in informal employment without any social protection, were deprived of their livelihoods. The poor, often self-employed, who constitute 75 per cent and 50 per cent of rural and urban households, respectively, have borne a disproportionate share of the burden. The impact on micro, small and medium enterprises, which account for 32 per cent of output and 24 per cent of employment in India, has been devastating. Thus, for poor households and small businesses, survival is at risk.

Healthcare for patients, except for those with Covid-19, has diminished in terms of both access and quality. In education, learning outcomes already poor will get worse as schools as colleges remain closed. In the economy, demand has dropped sharply as employment has contracted, while supply has been strangled by the massive reduction in output. Government revenues, for both Centre and states, have collapsed. And even if the lockdown is lifted altogether now, at best the economy will not grow during 2020-2021—and it will probably shrink.
THE LOSS OF life attributable to the virus must be situated in perspective. In India, on May 8th, total Covid-19 deaths were just about 2,000. In sharp contrast, 450,000 people die from tuberculosis every year. As many as 800,000 infants die every year, before reaching the age of one year, mostly due to easily preventable causes like pneumonia or diarrhoea. Another 1 million children die every year before they attain the age of five. These absolute numbers, and child mortality rates at more than 3 per cent, are the highest in the world. The economic consequences of the lockdown will make our children even more vulnerable.
Lockdowns, combined with mass testing, contact tracing, containment zones, mandatory quarantines, can only slow down the spread of infection. This might help in countries where public health facilities are robust, yet not adequate for large numbers when infections peak. But our public health system is poor and could never suffice for our large population if the pandemic were to spread. There is no vaccine yet. From development through trials to production will be at least a year, and far longer before it becomes available in sufficient quantities to suffice for our population. It is also essential to recognise that a lockdown is not a weapon in a war that can conquer or vanquish the microbe. The virus will be with us for some time to come, at least a year, if not longer, and there could be a spike in infections when the lockdown is eased, and such spikes may recur over time and across space. We have to learn to live with this reality and manage the virus as best as we can.
Healthcare for patients, except for those with Covid-19, has diminished. In education, learning outcomes will get worse. In the economy, demand has dropped sharply as employment has contracted, while supply has been strangled
It is now imperative to begin the process of exit from the lockdown. For one, it would enable the Government to find some balance between the twin objectives of saving lives and saving livelihoods. For another, it would help restart the economy, which has been almost completely shut down, and the collateral damage is bound to be far greater if the lockdown is extended.
Surprisingly enough, a calibrated, planned and phased exit could also help manage the spread of the virus. So far, morbidity and mortality associated with Covid-19 in India has been much lower than elsewhere in the world. This is possibly attributable to our immune systems, which have antibodies that could be effective in resisting the virus. After all, millions of migrants stranded in megacities or relief camps, crowded in cramped spaces—the polar opposite of social distancing—have not caught the virus through contagion in large numbers. It suggests there are already some elements of herd immunity in India that would grow stronger as the lockdown is progressively lifted.
This must happen at a much faster pace, because the present relaxations are nowhere near enough. It is time to let people get on with their lives. They must return to work and earn to feed their families. Migrants, who are the lifeblood of the urban services economy, should be able to resume work and reclaim their livelihoods. Farmers should no longer be hobbled with restrictions. Construction workers should return to their sites. Shopkeepers should be allowed to service their customers. Micro, small and medium enterprises, the heart of entrepreneurial India, need to be back in business. And factories need to hum with activity once again. Public transport has to be made functional. Hospitals should be accessible to patients for healthcare. Schools and colleges need to reopen for learning. The people and the economy cannot simply afford to allow the short-term effects of the past two months to turn into long-term consequences that could mortgage our future.
In an ideal world, lockdowns should be the exception and not the rule, specified in terms of geographical spaces to cities, containment zones and hotspots, or in terms of time schedules to restaurants, shopping malls, cinemas, tourism, international travel and congregations in public places.

/wp-content/uploads/2025/06/Cover-OpenMinds2025.jpg)












More Columns
Puri Marks Sixth Major Stampede of The Year Open
Under the sunlit skies, in the city of Copernicus Sabin Iqbal
EC uploads Bihar’s 2003 electoral roll to ease document submission Open