‘We may run out of staff sooner than oxygen’
A day in the life of a Covid ward in Bengaluru
/wp-content/uploads/2021/04/Thefrontline1.jpg)
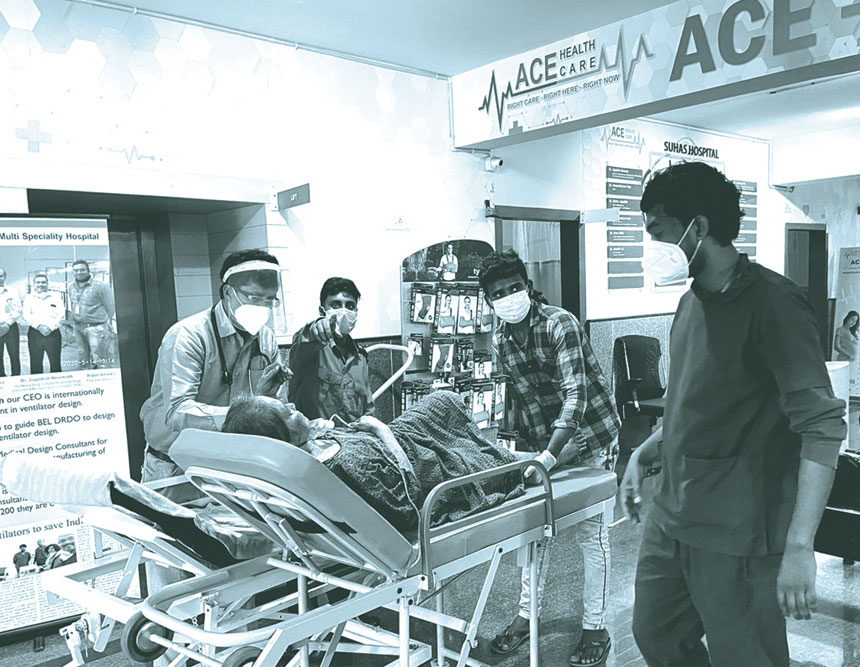
A patient is brought to ACE Suhas Hospital in Jigani on April 19
Five nurses have fallen ill. Two lab technicians have fallen ill. Three non-medical staff have fallen ill. ‘The toll we are taking is huge,’ reads Dr Jagadish Hiremath’s tweet looking for leads to urgently recruit nurses. Four hours later, he would be told that two doctors, exhibiting mild symptoms, are suspected positive, too. Thanks to their work, ‘the toll’, for the past couple of days, has not included any patient deaths at his 50-bed private hospital in Jigani, an industrial suburb to the south of Bengaluru. The hospital, which has allocated all its beds, including 10 in the ICU, to Covid-positive patients, is among the city’s last hopes against the daily mauling of the virus in its mutated, hungry new form, especially for those who failed to find a bed elsewhere, who were turned away because their prognosis was too dismal or the cost of treatment too high, who simply needed a reliable source of oxygen. An intensivist, Dr Hiremath, medical director of ACE Suhas Hospital, says he may run out of staff sooner than he will of oxygen or essential drugs. When he set up the hospital, he thought the proximity of large industrial units employing thousands would mean a steady stream of patients. Little did he imagine people from 55 kilometres away would queue up unbidden for a bed, dragging oxygen cylinders and knowing full well that they were at the edge of a very short cliff.
A year after nationwide public health efforts prioritised control over care, India leads the world in the daily average number of new infections reported. With one in every three infections worldwide reported from India, state-run and private hospitals alike are buckling at the knees. With limited ammunition and few new tricks in their arsenal, they must take down a moving target—a virus that is in the air, constantly mutating and choking the young and the old, the rich and the poor. “In the first wave, the Bruhat Bengaluru Mahanagara Palike (BBMP) played good cop bad cop with us very well. The people who asked us to allocate beds for Covid patients were the good cops and those who would give us the money were the bad cops. We have written off several lakh rupees. But given the expertise we have accumulated in dealing with Covid, we must step up to the occasion even if it means delays in payments, and below-par compensation by insurance companies,” Dr Hiremath says. The hospital treated over 230 Covid patients in 2020, including 80 in the ICU, and witnessed 17 deaths. This time round, he says, most patients are younger and therefore easier to treat, although there have been unexpected setbacks. Of the four patients he has lost to the second wave was a 36-year-old who succumbed to panic even as his body tried to staunch a cytokine storm for the second time since admission. He died in the ICU last week, even as his wife and child recovered in a ward upstairs. It was a heart attack that killed him—perhaps the shock of watching the man next to him and the one across die in quick succession had shaken his resolve to fight on. His family had been apprised of his progress, the lack of it, but the end came in the dead of the night, as if often does. With Covid, it is never a gentle ceasing. There are no memorably cohesive family moments. It is an echoless holler into the dark. And the shockwave of guilt and remorse that follows often shatters the survivors and sunders families. When a cancer survivor who had been in treatment for seven years contracted the infection from her son upon his return from overseas, and recently lost the final battle, the family erupted in an ugly spat in the hospital corridor, holding him responsible.

Sitting under the skylight on the lone bench in the first-floor corridor at noon, this heightened sense of mortality seems to disappear from the air momentarily. The summer wears on and ceiling fans click like clockwork. Nurses in scrubs and personal protective equipment (PPE) walk up and down, consulting their clipboards. They crouch and giggle behind the nurses’ station in a corner, where one of them, in her early-20s, checks her Instagram feed—her escape from reality. In the director’s room, Dr Hiremath inspects my PPE suit before I follow him and ACE Healthcare CEO Praveen Erappa on their rounds. Their phones don’t stop ringing—mostly calls, including from a local politician, desperately soliciting ICU beds—but they answer all the same, hoping it is a doctor or a nurse they can recruit. “There is no time for interviews. Just join right away,” Erappa tells a candidate over the phone. In a ward with three beds separated by beige curtains, a 28-year-old bank employee, let’s call him A Kumar, lies on his belly as per the doctor’s edict. It is his 15th day in hospital and his oxygen saturation has finally stabilised above 90. Loneliness and regret are writ large on his face. He had ignored his own symptoms when he brought his father and sister in for admission, says Erappa, who had luckily saved him a bed knowing he would be back. Kumar’s sister made a full recovery but his father has died, and he doesn’t know. “We are transparent with patients and we take care not to set unrealistic expectations. But the family has insisted that we keep the news of his father’s death from him. It is anybody’s guess how he will take it,” Dr Hiremath says. He asks Kumar to keep the oximeter clipped on at all times. Devices measuring his blood pressure, oxygen saturation and pulse are connected to a remote monitoring system called Dozee, designed by an Indian startup. Periodic reports and daily summaries are sent over WhatsApp to doctors and the app on their phone raises an alarm when a patient’s vitals are critical. “Without technology, managing this pandemic would have been impossible for a small hospital,” Dr Hiremath says. He has also been able to leverage his contacts for critical medical supplies, especially oxygen cylinders. The hospital has been going through 30 jumbo cylinders—each with a capacity of 7,000 litres—in a day and barely manages to meet its requirement despite distributing the demand among three suppliers and often sending its own ambulances to fetch cylinders from warehouses.
‘Remdesivir is the new ganja. Suppliers are demanding Rs 35,000 in cash per vial for what should cost no more than Rs 2,500. And this, for a drug that is not even proven to be effective in treating Covid. Yet, some patients ask for it, just like some ask for a guarantee that they will go back home alive,’
says Praveen Erappa, CEO, Ace Healthcare
In the basement, past the diagnostics lab and the vaccination station, the erstwhile optical department, with eyeglasses still on display on the wall, now stores empty cylinders. A tempo has arrived from Kaveri Gas Products to pick up nine cylinders and deliver as many filled ones, which are then carefully stowed in a back room. The hospital has not had much luck with liquid oxygen tanks, which it has found to be prone to leaks. While the state health minister has spoken of setting up an oxygen war room to divert the supply of locally produced oxygen from industrial to medical use, shortages loom large for most hospitals in the city. In fact, a patient has just been wheeled in from a bigger hospital that closed down yesterday upon running out of oxygen. He arrives on a stretcher in an ACE Suhas ambulance, barely conscious, his son heaving the oxygen cylinder into the elevator with him. According to the front desk, there have been 100-plus walk-ins until 4PM today, including 25 who came to be vaccinated. The hospital has capped the number of jabs at 50 per day, but there are never enough takers. “What people come asking for is remdesivir. It’s the new ganja. Suppliers are demanding Rs 35,000 in cash per vial for what should cost no more than Rs 2,500. And this, for a drug that is not even proven to be effective. When a patient insists, we try to source directly from pharma companies,” says Erappa. Admissions are strictly by prior telephonic confirmation, with just one bed reserved for the hospital’s own staff in case one of them should require it. There are seminar rooms, recovery areas and other spaces they could quickly turn into ICUs if required, but unreliable oxygen supply is a key limiting factor. “When a patient is admitted, the first thing the family asks is, can you give us a guarantee for his life? How can we?” Erappa says.
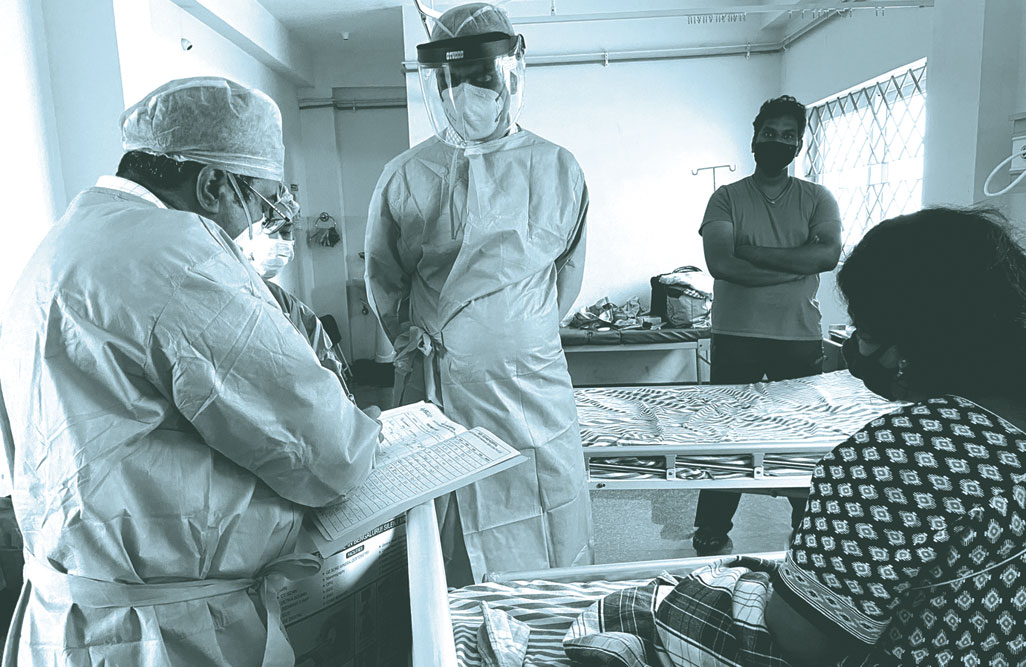
The three floors of the hospital house patients who have all experienced life differently. Some played fast and loose, infecting their entire families; others doggedly cling to a culture of entitlement, possibly to feel some sense of personal agency. In a special ward on the third floor, a woman points to the empty bed at some distance from her own and says she could not sleep a wink because of the constant click of sobs from the widow of the 36-year-old who had died in the ICU days ago. “I have a sore throat because I did not get warm water to drink yesterday,” the woman complains in Hindi. Everyone is trying to escape the script in their own way, some with inveterate optimism, others by wielding their privilege and stacks of cash. “Patients want services. Some are demanding things and attention as though there isn’t a pandemic raging. One patient said he will pay Rs 20,000 extra per day if we could devote a senior staff member entirely to his care,” says Dr Hiremath.
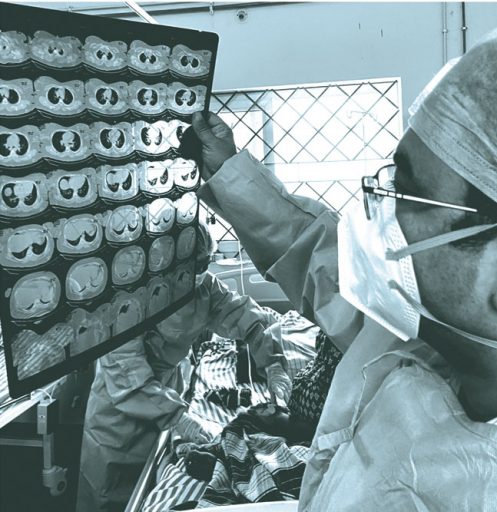
Patients can be obdurate even when death stares them in the face. Recovering in another room on the third floor is a young mother to a five-month-old who had refused treatment as she wanted to continue breastfeeding. She is back in hospital with a high fever and incessant vomiting. “She does not look good,” Dr Hiremath says, but a look at her CT scan assures him her lungs are not in danger. Two weeks have passed since she first reported sick, but it is only over the past five days that she has been on antivirals and steroids.
In another case of recurrence soon after discharge, the patient’s low thyroid levels and obesity—an important comorbidity that does not get enough attention, Dr Hiremath says—came into play. “She has been incredibly positive throughout and we are ready to discharge her.” He demonstrates breathing exercises to the patient in an airy room where the tables are strewn with the detritus of illness—toiletries, towels, blankets, chargers, clothing. “There is a certain psychosomatic component we are missing. Young people who are panicking are developing serious symptoms. It is not uncommon to have patients go straight from ‘I can take care of myself at home’ to ‘Please, don’t let me die’,” he says.
‘For Covid hospitals, 8PM is the hour of dread. Across the world, most cytokine storms seem to occur at night. Weathering one is hard—even with the best medical care. While we are better prepared for the second wave, and know largely what to expect, we cannot predict outcomes for every patient’
Dr Jagadish Hiremath, Medical Director, Ace Suhas Hospital
A young doctor, walking like a space-age pharaoh in a PPE suit, mans the ICU, a set of rooms in one wing of the second floor that is the demarcation point for the critically ill. “We have been taking cases that even advanced tertiary care hospitals have turned away,” says 31-year-old surgeon and Covid specialist Dr Farman Ali. Most beds have the curtains drawn around them. The first bed is occupied by a 31-year-old whose lungs are over 75 per cent impacted and whose vitals crash the moment oxygen support is withdrawn. His family—two men in football jerseys who are pacing up and down making calls—is hoping to move him to a larger hospital with ECMO, an intra-aortic balloon pump and other advanced facilities, but the waitlists at Manipal, Narayana or Global Hospitals are not getting much shorter. In a far corner of the ICU, a patient who was brought in with extremely high blood sugar five days ago mumbles deliriously. Dr Ali says he may be moved to a ward after another day of observation: his diabetes has been brought under control and his lungs are almost clear of the virus. Another patient with renal failure is all set to undergo Sustained Low Efficiency Dialysis later in the evening—a procedure most hospitals elect not to perform on Covid patients, since the dialysis equipment used on them, costing about Rs 10-14 lakh, cannot be re-used on others. “We have managed the most serious of cases but ICU psychosis is a real and present danger and we try to move patients out to wards as soon as they are stable,” says Dr Ali, who also runs an agency for homecare that has treated over 800 patients in the past year.

Back at Erappa’s office, a young pharmacist and a front office staffer come asking for some time off. They fear there is going to be another lockdown in Bengaluru, and they want to return to their village. Erappa shakes his head. The hospital has ended up having to hike salaries of housekeeping staff to Rs 30,000 and beyond—more than what some junior nurses draw—and lost its entire dialysis team to poaching by a healthcare company. “Finding a good medical worker today is like finding a moth in the dark,” Erappa says. A call from Dr Chandra Mohan, the other ICU doctor on duty, sends him dashing to the front office. A Trinity Central Hospital ambulance is parked outside and a 92-year-old patient on oxygen has been wheeled out. The elevator is tiny and will only fit the in-house stretcher, so three men, including a young casualty doctor in scrubs, a security guard and the ambulance driver haul her on to it. None of them wears a PPE.
There are more ambulance sirens ringing in the bruising dusk. Eight in the evening is the hour of dread. It is when the specialists on the ground floor wind up their OPDs and the staff prepares for the night shift. There is something stark and final about a Covid hospital after dark. The world over, cytokine storms seem to hit at night, says Dr Hiremath. “The first signs of tachypnea—fast and shallow breathing, more than 25 times a minute—indicates the beginning of a storm, and once it starts raging, there is precious little we can do.” Watching meal trays being delivered and hearing the occasional cough pierce the evening, I imagine the internal monologues of the patients. How many of them think themselves safe in a medical oasis? And how many must be overcome with debilitating dread, waiting for a horrifying confirmation that they could end up as a statistic?

/wp-content/uploads/2025/07/Cover-Shubman-Gill-1.jpg)














More Columns
‘Fuel to Air India plane was cut off before crash’ Open
Shubhanshu Shukla Return Date Set For July 14 Open
Rhythm Streets Aditya Mani Jha