Vaccinate and be Saved
So long and science is still the salvation
 Shahid Jameel
Shahid Jameel
 Shahid Jameel
|
03 Sep, 2021
Shahid Jameel
|
03 Sep, 2021
(Illustration: Saurabh Singh)
REPORTS BEGAN coming in around December 2019 of a new disease that started as a cluster of unusual pneumonia cases in Wuhan, China. The disease quickly went global and was declared a pandemic on March 11th, 2020. It was called coronavirus infectious disease 2019 (or Covid-19) for the causative agent—a coronavirus—which was itself christened severe acute respiratory syndrome coronavirus-2 (or SARS-CoV-2) based on the respiratory disease it caused and its similarity to another virus (SARS-CoV) that had emerged in late 2002. As of August 24th, over 213 million people had been confirmed with SARS-CoV-2 infections and over 4.4 million had died worldwide. Both numbers are likely to be underestimates.
The ongoing pandemic has impacted our lives in so many ways that when historians write about the modern world, time would be divided into pre and post-Covid-19.
Where Did It Come From?
Everything comes from somewhere. And so did SARS-CoV-2.
Viruses comprise only about 15 per cent of human pathogens (or disease-causing agents) but almost 50 per cent of new and emerging pathogens are viruses. And about 75 per cent of all emerging viruses are zoonoses, that is, they come into the human population from animals. While words like ‘spillover’ and ‘jump’ are used to describe this transfer, it is simply a matter of opportunity. The key driver for this transfer is increased human-animal contact caused by deforestation and loss of wild animal habitats. Virus transmission risk is highest from abundant animal species that have adapted to human-dominated landscapes. Bats and rodents possess the highest mammalian species richness and the highest diversity of zoonotic viruses, and are natural donors. Humans as the most abundant species on earth are an obvious target. The virus can ‘jump’ directly into humans or come through another ‘amplifier’ animal species. A Nipah outbreak in Malaysia in September 1998 was traced to the virus spillover into humans not from bats, but through pigs. However, several outbreaks in Bangladesh in the first decade of this century were traced to direct transmission from bats to humans. It’s all about opportunity.
Like for several other (corona)viruses, evidence suggests that SARS-CoV-2 also came from bats. How it was transmitted to humans—Directly? Through an intermediate animal species? Did it go from a bat to a lab where it was tweaked by scientists and then leaked either accidentally or intentionally?—remains to be established. While several arguments have been put forward for a ‘lab leak’, current scientific evidence, which includes genetics and phylogeny, still favours a jump from bats to humans, either directly or through a yet to be discovered animal species. Over 400 bat samples collected from the Yunnan province in China between May 2019 and November 2020 revealed 24 full-length coronavirus genomes, including four novel SARS-CoV-2-related and three SARS-CoV related viruses. The virus obtained from Rhinolophus pusillus, also called the least horseshoe bat, a species endemic to Southeast Asia including Northeast India, was the closest relative of SARS-CoV-2 in most of the genome, except for a more divergent spike gene. Bat coronaviruses are remarkably diverse and include close relatives of both SARS-CoV-2 and SARS-CoV.
Though there is little scientific evidence at this time to support the claim that a virus was modified in the lab and leaked from it, gain-of-function studies and accidental releases have taken place in the past. Resolving this debate would require China to make hospital and laboratory records, computers, freezers, etcetera available for international inspection. In the present geopolitical environment that is unlikely to happen.
India: A Retrospective
As of August 24th, India has over 3.25 crore confirmed Covid-19 cases and 4.35 lakh deaths.The first case of SARS-CoV-2 infection in India was registered on January 30th, 2020 in a 27-year-old medical student who returned home to Thrissur in Kerala from Wuhan. More cases started appearing in early March 2020. Let us summarise the key events since then (see figure titled ‘Covid-19 in India’).
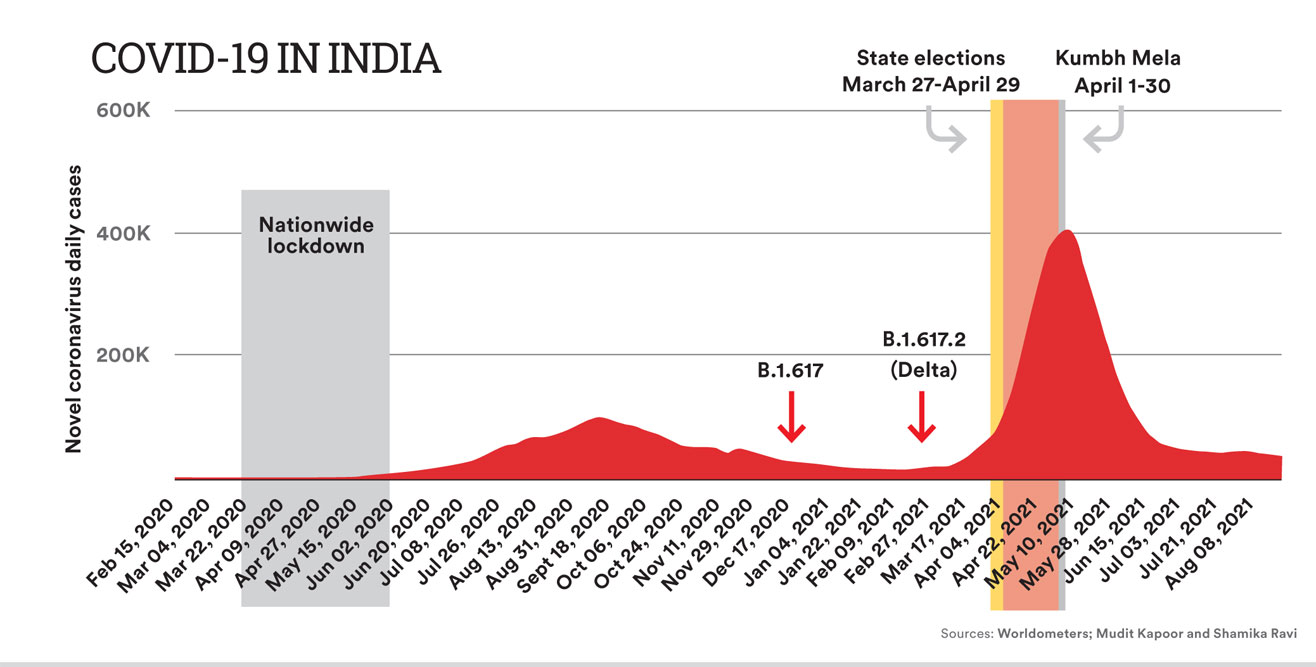
India announced a national lockdown on March 24th, 2020 with 534 confirmed cases and 11 deaths. This continued till May 31st, 2020, by when there were 1,90,609 confirmed cases and 5,426 deaths. A steady rise in cases took place till mid-September 2020 to almost 93,000 cases per day, followed by a gradual decline to about 11,000 daily cases by mid-February 2021. This constituted the first wave in India. During April, cases rose exponentially to reach almost 4 lakh daily by early May, receding thereafter to a new set point of about 35,000-40,000 cases per day. This became the devastating second wave.
Was the nationwide lockdown successful? Data show the average growth rate of active cases fell rapidly during the first phase of the lockdown but slowed down thereafter. This, together with the associated economic and livelihood costs, encouraged the Government to relax the lockdown even when daily cases were rising. While the sudden lockdown had associated economic and livelihood costs, it ‘flattened the curve’ giving enough time for healthcare services to be ramped up.
A decline in cases during mid-September 2020 to mid-February 2021 led to complacency at the individual, government and policy levels. New and more infectious virus variants were also developing during this time. The B.1.617 variant was first seen in genome sequencing results from Maharashtra in December 2020 and by February it had further mutated into the B.1.617.2 lineage, now known as the delta variant. The delta variant got momentum from superspreader events such as the state Assembly elections and the Kumbh Mela that brought very large numbers of people who did not follow masking or distancing protocols together in one place. Further, since only 0.3 per cent of the population had received one dose of vaccine by the end of February, the population had no vaccine-mediated protection. This resulted in a huge second wave, a collapse of the healthcare system and very large numbers of deaths.
A recent study has estimated 2.5-2.8 million Covid-19 deaths in India just during the second wave. Overall, India’s Covid-19 mortality is estimated to be 7-8 times higher than the official numbers.
The Delta Deluge
India’s massive second wave was due to the delta variant, which has now been reported in 115 countries. This spread very quickly across India and to other parts of the world by outcompeting other variants. Following its appearance in February, the delta variant was found in over 80 per cent of new infections in India by April and in 100 per cent by July. In Europe, it comprised less than 5 per cent of new infections in April but now causes over 95 per cent of infections. In North America, it has expanded from about 1 per cent in May to 97 per cent at this time. Africa and South America where the beta and gamma variants remain dominant, respectively, don’t so far show any visible spread of the delta variant. Such selective geographic spread is another example of opportunity.
Why did the delta variant spread so quickly? The R0 (called ‘R naught’) represents the number of new infections that could stem from a single case. It was estimated to be 2-3 for the original virus but is 5-10 for the delta variant, which makes it the most transmissible variant yet. This high infectivity is traced to the synergistic action of key spike protein mutations. A mutation called L452R allows the virus to bind better to the ACE2 receptor on cells. Another mutation called P681R allows more efficient cleavage of the spike into S1 and S2, a step that is necessary for a virus’ entry into cells. Yet another mutation called T478K allows the virus to escape some pre-existing virus-neutralising antibodies. Thus, the delta variant binds, infects and evades better, producing more virus particles in infected people, which makes it easier to transmit and thus more infectious. It also appears to cause more severe disease and increased hospitalisation. Public Health England reported that the risk of hospitalisation from the delta variant increases by 32 to 289 per cent compared with the alpha variant. High transmission rates overwhelm the public health system and make the variant more deadly.
Vaccines and Vaccinations
Vaccines normally require years to develop, but safe and effective Covid-19 vaccines have been produced in record time. So far eight vaccines have received full use approval, 12 have early or limited use approval, about 100 are in clinical trials on humans, and over 75 vaccines are undergoing preclinical testing in animals. Multiple platforms have been used, which include inactivated viruses, viral vectors, mRNA and DNA. At least 200 countries have started vaccinating against Covid-19, but problems of access and equity remain.
Seven vaccines have been approved for use in India, of which three—Covaxin (Bharat Biotech), Covishield (Serum Institute of India) and ZyCoV-D (Zydus Cadila)—are made locally. The others are mRNA-1273 (Moderna, the US), AZD122 (AstraZeneca, the UK), Sputnik V (Gamaleya Institute, Russia) and Ad26.COV2.S (Janssen, the US). Of the 59.1 crore doses administered in India till recently, Covishield accounts for 87.5 per cent, Covaxin for 12.4 per cent and Sputnik for 0.1 per cent. Although India has administered the world’s second highest number of vaccine doses, only 33 per cent people have received one vaccine dose and only 9.5 per cent are fully immunised. Over the past few weeks, about 14.5 crore doses have been administered, averaging about 50 lakh doses per day. This rate needs to double, but the domestic availability of doses remains a challenge. Between May and June, the Indian Government slashed its own projections of vaccine availability from 216.6 crore to 135 crore doses.
The Delta variant was found in over 80 per cent of new infections in India by April and in 100 per cent by July. In Europe it comprised less than 5 per cent of new infections in April but now causes over 95 per cent of infections. In North America it has expanded from about 1 per cent in May to 97 per cent. Africa and South America don’t so far show any visible spread of this variant
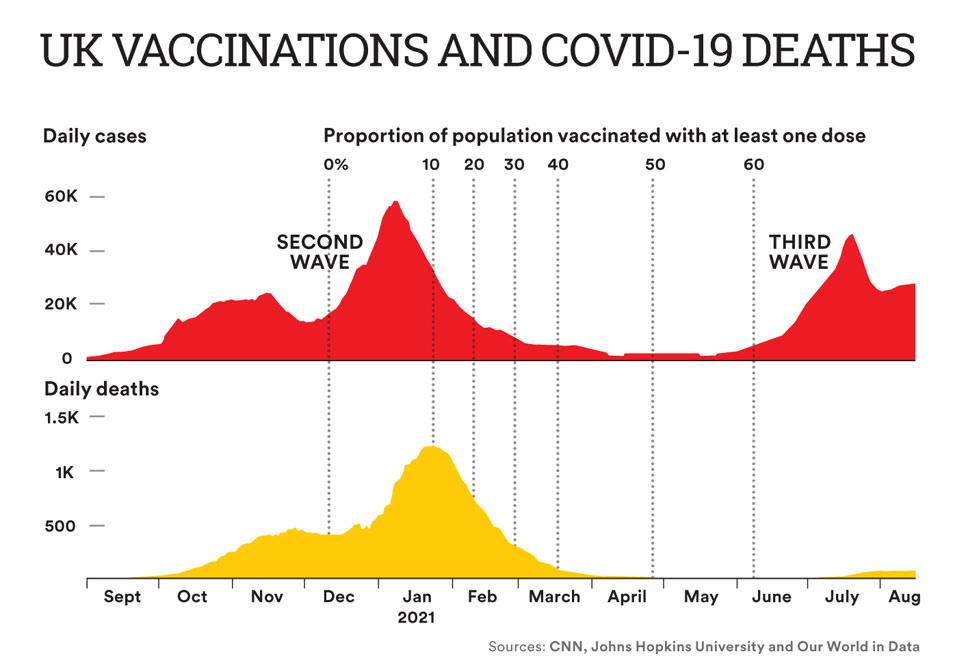
Do vaccines protect against the more transmissible delta variant? Several studies, including some from India, show that while vaccines offer variable protection against symptomatic infection, all vaccines protect very well from severe disease, hospitalisation and mortality. At least four studies from the UK show the Pfizer-BioNTech and AstraZeneca vaccines to be about 90 per cent effective against hospitalisation from the delta variant. With increased vaccinations, the UK has shown a significant reduction in mortality (see figure titled ‘UK Vaccinations and Covid-19 deaths’). In the US, of the 164 million vaccinated people, only 0.077 per cent tested positive for breakthrough infections and 0.001 per cent died of Covid-19.
Will There Be a Third Wave in India?
A big third wave is unlikely to happen in India. Results from the 4th National Serosurvey conducted during June and July show about two-thirds of Indians to have antibodies to SARS-CoV-2. In urban centres this number would be higher. For example, results from Delhi show 86 per cent people to have antibodies. This means that a very large fraction of the population has already been exposed to the virus and would be protected from symptomatic infection, severe disease and hospitalisation.
But this does not mean that we have achieved ‘herd immunity’. First, the exposed people would not be evenly distributed across the country and there would still be pockets of more susceptible people. Kerala with only 44 per cent seroprevalence is one example, which continues to show high number of daily cases. Secondly, with the highly infectious delta variant the threshold of herd immunity would be much higher.
A third wave will depend upon several factors. Individual behavior is important: how well people follow Covid-19 protocols of using masks, avoiding crowds, etcetera; how quickly we can vaccinate susceptible populations would also be crucial. Finally, it remains to be seen whether more infectious variants will emerge that evade acquired immunity. At this time, it would be prudent for individuals to exercise caution and for governments to be prepared.
When Will the Pandemic End?
In his speech at the 138th International Olympic Committee Session in Tokyo on July 21, World Health Organization Director-General Tedros Ghebreyesus said, “I am often asked when the pandemic will end. My answer is equally simple: the pandemic will end when the world chooses to end it. We have the tools to prevent transmission and save lives.”
There is no good answer to this question because there is no one definition of what the end of the pandemic means. A pandemic is a global crisis and unless the virus is controlled globally, it’s not going away. When the worldwide spread of a disease is brought under control and it persists globally at expected or normal levels, it becomes endemic. At that stage, SARS-CoV-2 will become a circulating and inconsequential virus because we will build immunity against it.
Science has provided the tools to quickly detect the virus, sequence its genome for a better understanding and vaccines to develop immunity. For the first time in the history of human infectious diseases we have the opportunity to end a pandemic with vaccines.
Let us not waste this historic opportunity.














More Columns
Art of Love Nandini Nair
Fruit of the Nation Madhavankutty Pillai
Ladakh: Magic Mountain Abhilasha Ojha